Personalized Knee Exoskeletons: Bringing Rehab Home with an Adjustable, Patient-Friendly Design
Recovery from knee injuries ACL tears, meniscus damage, osteoarthritis flares, or post-replacement surgery often stalls when patients can’t attend frequent clinic sessions. Traditional therapy relies on supervised machines or manual assistance, but what if the support could travel with the user? At Nazarbayev University’s Center for Excellence in Medical Robotics and Rehabilitation (CEMRR), engineers have prototyped a mobile knee exoskeleton that brings controlled, adjustable assistance directly to the home or bedside.
The device is designed as a lightweight, wearable orthotic that assists flexion/extension while offloading stress on the joint. It provides graduated support passive when the patient needs rest, active when they’re ready to push helping rebuild strength, range, and confidence without constant therapist supervision.
Digital-First Design: From CAD to Clinical Reality
The entire development unfolded in Autodesk Fusion 360, a modern CAD platform that let the team model every component in 3D, simulate assembly, check clearances, and predict interactions before cutting a single piece of material. This digital workflow caught misalignments early, slashed prototyping errors, and accelerated the leap from concept sketch to physical prototype.
The core goal was clinical utility: create an assistive mechanism that safely absorbs load, guides movement, and progressively restores mobility. Beyond mechanics, the designers prioritized psychological comfort—patients often feel vulnerable during recovery. A device that feels secure and supportive builds trust, reduces fear of movement, and boosts adherence.
Universal Fit: One Device, Many Patients
From day one, the exoskeleton was engineered for versatility. Rigid, fixed-geometry braces limit use; this one adjusts along all three axes (X mediolateral width, Y anteroposterior depth, Z vertical height). The result accommodates adolescents through adults, varying leg lengths, muscle bulk, and body types, eliminating the need for custom builds per patient.
Upper attachment uses a wide thigh strap for even pressure distribution across soft tissues. Lower attachment grips the shin and calf with rigid Y-axis depth adjustment for limb shape conformity, plus free Z-axis play that lets the mechanism self-align during flexion/extension. This passive compliance follows the knee’s natural trajectory, minimizing shear forces and discomfort.
Engraved scales on steel guide tubes allow quick, repeatable setup, therapists note settings once, then reproduce them exactly in every session. Symmetry is maintained: X-axis width links upper and lower sections, with optional spacers fine-tuning motor/bearing alignment for individual leg proportions.
Smart Material Choices: Balancing Speed, Strength, and Future Weight Savings
Prototyping demanded fast iteration and lab-friendly fabrication. The team chose:
3D-printed ABS plastic for adjustable blocks and non-load-bearing parts. ABS offers good strength (30–48 MPa tensile), ductility (10–30% elongation), and impact resistance ideal for rapid design-print-test cycles. Complex shapes print quickly and swap easily during refinement.
Laser-cut steel plates and tubes for load-bearing mounts, guides, and frames. Steel’s high yield strength (~250–350 MPa) and rigidity (200 GPa modulus) handle dynamic forces from motor torque and patient weight without deformation.
This hybrid kept costs low and assembly swift no exotic materials or outsourced machining required. Future iterations will shift to anodized 6061-T6 aluminum profiles: roughly one-third the density of steel, solid yield strength (~276 MPa), excellent fatigue resistance, and corrosion protection after anodizing. The upgrade promises a noticeably lighter device without sacrificing durability—critical for all-day wear or home use.
Real-World Fit: How It Looks and Feels on the Leg
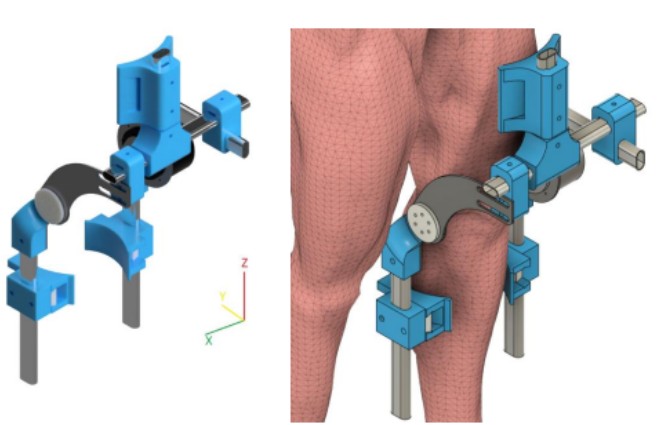
Isometric CAD renderings (anterior left/right views) show clean spatial organization: motor positioned laterally, straps wide and padded, adjustments intuitive. Overlaid on an anatomical model, the exoskeleton hugs the femur and tibia contours naturally no awkward bulk or protrusion.
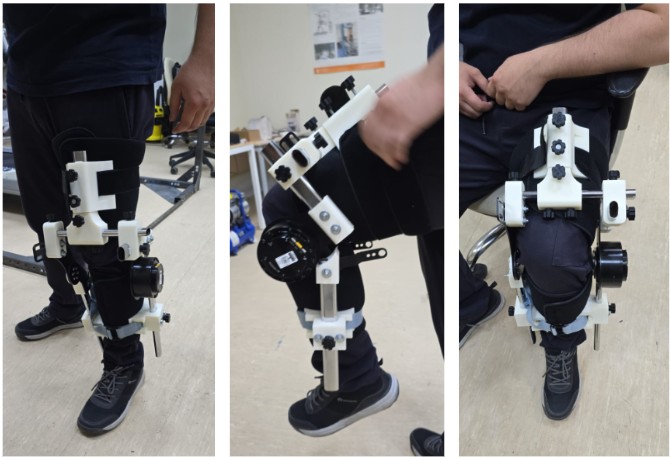
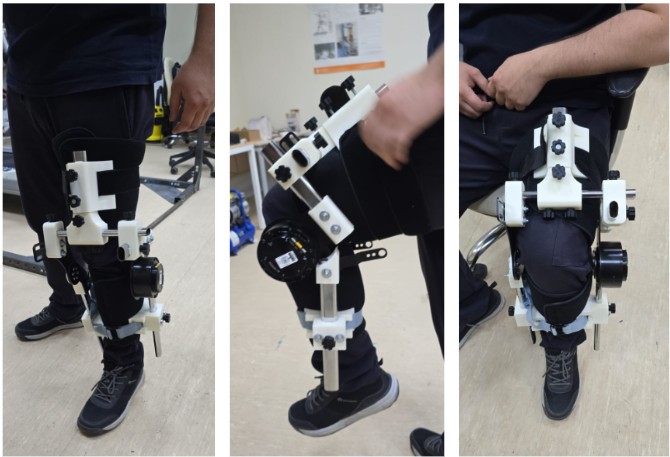
Photos of the assembled prototype on a standing subject confirm snug, symmetric fit. Wide straps with soft padding distribute pressure evenly; no shifting or twisting occurs under static load. The motor and guides stay compact, preserving natural stance and bilateral balance.
In suspended-leg mode (limb hanging freely), images reveal precise axis alignment with the anatomical knee center essential to avoid unwanted tissue strain. Z-axis free play allows smooth self-alignment through the full range; no binding or resistance disrupts motion.
Sitting-position shots (common for most rehab exercises) highlight stability during flexion/extension. Even at deep angles, the device remains secure and unobtrusive. Patients can perform standard therapy movements—controlled bends, holds, or assisted extensions without the exoskeleton interfering or slipping.
The Bigger Picture
This mobile knee exoskeleton proves that high-quality rehab hardware doesn’t require massive budgets or factories. Using accessible tools (Fusion 360, 3D printing, laser-cut steel), the team built a versatile, ergonomic prototype that prioritizes patient comfort, repeatability, and clinical practicality.
Next steps include sensor integration (position, torque, IMUs), adaptive control algorithms, and lightweight aluminum/composite upgrades. Clinical pilots will test safety, usability, and functional gains (range, strength, pain reduction) in real patients.
For millions recovering from knee trauma especially in regions with limited clinic access—this kind of device could shift rehab from appointment-dependent to daily, on-demand support. When the exoskeleton fits like it belongs on the leg, recovery stops feeling like a chore and starts feeling possible.